New Studies Show Impact of Endothelial Dysfunction on Heart Failure with Preserved vs
- heartlung
- Jan 16, 2023
- 3 min read
Reduced Ejection Fraction, Taurine Supplementation Reduce Endothelial Dysfunction
Heart Vessels. 2018 Feb 1. doi: 10.1007/s00380-018-1128-2. [Epub ahead of print] Heart failure with preserved vs reduced ejection fraction following cardiac rehabilitation: impact of endothelial function. Tanaka S1, Sanuki Y2, Ozumi K2, Harada T2, Tasaki H2. Author information 1Department of Cardiovascular Medicine, Kitakyushu Municipal Yahata Hospital, 4-18-1 Nishihon-machi, Yahatahigashi-ku, Kitakyushu, 805-0061, Japan. sayatanaka@me.com.2Department of Cardiovascular Medicine, Kitakyushu Municipal Yahata Hospital, 4-18-1 Nishihon-machi, Yahatahigashi-ku, Kitakyushu, 805-0061, Japan. Abstract There is no proven therapy for heart failure with preserved ejection fraction (HFpEF). Research has shown beneficial responses to cardiac rehabilitation (CR) among HF patients. To date, there are no reports comparing those responses between patients with HFpEF and those with reduced ejection fraction (HFrEF). The purpose of this study was to compare responses to CR in patients with HFpEF versus those with HFrEF. We included 78 consecutive patients (mean age 69 ± 15 years; 80% male) with HF in our CR unit who underwent cardiopulmonary exercise testing and brachial artery flow-mediated dilation (FMD) testing pre- and 5 months post-CR. Patients were judged as HFpEF (n = 40) or HFrEF (n = 38) using a left ventricular ejection fraction (LVEF) cut-off of 50%, and endothelial dysfunction was defined as FMD ≤ 5.0%. Following 155 ± 11 days and 44 ± 8 sessions, peak oxygen uptake ([Formula: see text]) and plasma B-type natriuretic peptide concentrations improved significantly in both groups. The percentage change in peak [Formula: see text] of HFrEF patients was significantly greater than compared with the HFpEF patients (P < 0.01). To further investigate whether a combination of LVEF and FMD values predicts the effect of CR, we divided patients into four groups according to LVEF of 50% and FMD of 50%. Post hoc analysis showed a significant difference between HFrEF patients without endothelial dysfunction and HFpEF patients with endothelial dysfunction (P = 0.01). In conclusion, although CR improves prognosis in HF patients, a larger effect can be expected in HFrEF patients than in HFpEF patients, and endothelial function may enhance the effect. KEYWORDS: Cardiac rehabilitation; Flow-mediated dilation; Heart failure with preserved ejection fraction; Heart failure with reduced ejection fraction
Eur J Nutr. 2018 Jan 27. doi: 10.1007/s00394-018-1616-2. [Epub ahead of print]
Taurine supplementation prevents endothelial dysfunction and attenuates structural changes in aortas from hypothalamic obese rats.
Leão VF1, Ferreira LLDM1, Melo CM1, Bonfleur ML2, da Silva LL1, Carneiro EM3, Raimundo JM1, Ribeiro RA4.
Author information 1Universidade Federal do Rio de Janeiro, NUPEM, Campus UFRJ-Macaé, Avenida São José do Barreto, 764, Macaé, RJ, CEP 27965-045, Brazil.2Centro de Ciências Biológicas e da Saúde, Universidade Estadual do Oeste do Paraná (UNIOESTE), Cascavel, PR, Brazil.3Departamento de Biologia Estrutural e Funcional, Instituto de Biologia, Universidade Estadual de Campinas, Campinas, SP, Brazil.4Universidade Federal do Rio de Janeiro, NUPEM, Campus UFRJ-Macaé, Avenida São José do Barreto, 764, Macaé, RJ, CEP 27965-045, Brazil. rosaneribeirobio@gmail.com.
Abstract PURPOSE: Obesity predisposes to cardiovascular and metabolic diseases. The amino acid, L-taurine (Tau), regulates glucose and lipid homeostasis and vascular function. Here we investigated whether Tau supplementation prevents endothelial dysfunction in the thoracic aortas of monosodium glutamate-induced obese (MSG) rats. METHODS: Male rats received subcutaneous injections of MSG (4 mg/kg body weight/day) or saline (control group, CTL) during the first five days of life. From 21 to 150 days of age, the rats were distributed into the groups: CTL, MSG, and CTL and MSG supplemented with 2.5% Tau in their drinking water (CTAU and MTAU). RESULTS: At 150-days old, MSG rats presented massive abdominal fat deposition, hypertriglyceridemia, hyperinsulinemia, glucose intolerance and high plasma levels of malondialdehyde (MDA), a lipid peroxidation marker. Tau supplementation attenuated fat accumulation in perigonadal adipose tissue and prevented the increase in triglycerides and MDA plasma levels. Aortic rings of MSG rats presented reduced vasodilation in response to acetylcholine (ACh). No modifications in insulin-induced vasodilatation, or Akt and eNOS phosphorylation, were observed in MSG aortas; thoracic aortas from MSG rats presented reduced tunica media thickness, with a lower aortic wall thickness/lumen diameter ratio and decreased total collagen content. Tau supplementation restored ACh-induced vasodilation and collagen content. CONCLUSIONS: Our study presents the first evidence that Tau prevents disruptions in vascular reactivity and in extracellular matrix composition in thoracic aortas of MSG-obese rats. The vascular protective actions of Tau may be linked to reduced lipid peroxidation and a reduction in cardiovascular risk factors, such as abdominal fat and hypertriglyceridemia.
KEYWORDS: Aortic morphology; Endothelial dysfunction; Lipid peroxidation; Taurine
Endothelial Function Scientific Update Sponsored by Endothelix Inc.
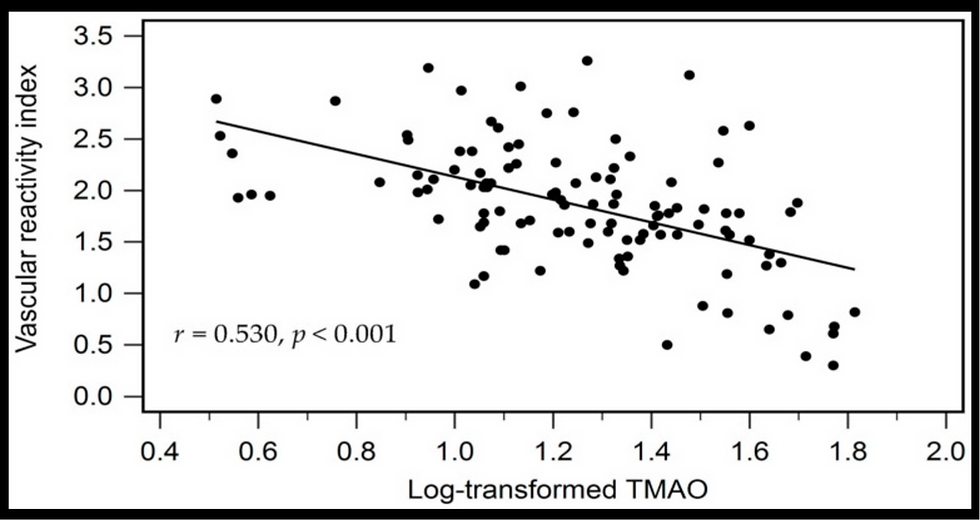
![Lipoprotein(a) levels predict endothelial dysfunction in maintenance hemodialysis patients: evidence from [VENDYS] vascular reactivity index assessment](https://static.wixstatic.com/media/dac531_5285607cc591409a9d83746f042af7c6~mv2.png/v1/fill/w_980,h_980,al_c,q_90,usm_0.66_1.00_0.01,enc_avif,quality_auto/dac531_5285607cc591409a9d83746f042af7c6~mv2.png)

Comments