Dr. Fuster’s top 100 picks from JACC 2020 and Dr. Naghavi’s top 5
- heartlung
- Jan 16, 2023
- 7 min read
Updated: Jan 18, 2023


JACC Editor-in-Chief’s Top 100 Picks Valentin Fuster, MD, PhD Each week, I record audio summaries for every paper in JACC, as well as an issue summary. Although this process is quite time-consuming, I have become familiar with every paper that we publish. Thus, I have personally selected the top 100 papers (both Original Investigations and Review Articles) from the distinct specialties each year. In addition to my personal choices, I have included papers that have been the most accessed or downloaded on our websites, as well as those selected by the JACC Editorial Board members. In order to present the full breadth of this important research in a consumable fashion, we will present these abstracts in this issue of JACC, as well as their Central Illustrations.

Scientific Updates’ Top 5 of the 100
Picked by Dr. Naghavi

Morteza Naghavi, MD Founder of SHAPE and President of American Heart Technologies
Incorporating Coronary Calcification Into Pre-Test Assessment of the Likelihood of Coronary Artery Disease Simon Winther MD, PhDa Samuel EmilSchmidt MSc, PhDb Thomas Mayrhofer PhDcd Hans Erik Bøtker MD, DMSci, PhDe Udo Hoffmann MD, MPHc Pamela S. Douglas MDf William Wijns MD, PhDgh Jeroen Bax MD, PhDi Louise Nissen MD, PhDa Vibeke Lynggaard PhDa Jens Juel Christiansen MD, PhDj Antti Saraste MD, PhDkl Morten Bøttcher MD, PhDa Juhani Knuuti MD, PhDkl Background The prevalence of obstructive coronary artery disease (CAD) in symptomatic patients referred for diagnostic testing has declined, warranting optimization of individualized diagnostic strategies. Objectives This study sought to present a simple, clinically applicable tool enabling estimation of the likelihood of obstructive CAD by combining a pre-test probability (PTP) model (Diamond-Forrester approach using sex, age, and symptoms) with clinical risk factors and coronary artery calcium score (CACS). Methods The new tool was developed in a cohort of symptomatic patients (n = 41,177) referred for diagnostic testing. The risk factor–weighted clinical likelihood (RF-CL) was calculated through PTP and risk factors, while the CACS–weighted clinical likelihood (CACS-CL) added CACS. The 2 calculation models were validated in European and North American cohorts (n = 15,411) and compared with a recently updated PTP table. Results The RF-CL and CACS-CL models predicted the prevalence of obstructive CAD more accurately in the validation cohorts than the PTP model, and markedly increased the area under the receiver-operating characteristic curves of obstructive CAD: for the PTP model, 72 (95% confidence intervals [CI]: 71 to 74); for the RF-CL model, 75 (95% CI: 74 to 76); and for the CACS-CL model, 85 (95% CI: 84 to 86). In total, 38% of the patients in the RF-CL group and 54% in the CACS-CL group were categorized as having a low clinical likelihood of CAD, as compared with 11% with the PTP model. Conclusions A simple risk factor and CACS-CL tool enables improved prediction and discrimination of patients with suspected obstructive CAD. The tool empowers reclassification of patients to low likelihood of CAD, who need no further testing.

Percutaneous Coronary Intervention for Vulnerable [Non-Obstructive] Coronary Atherosclerotic Plaque Gregg W.Stone MDab Akiko Maehara MDbc Ziad A. Ali MD, DPhilbc Claes Held MD, PhDd Mitsuaki Matsumura BSb Lars Kjøller-Hansen MD, DMSce Hans Erik Bøtker MD, PhD, DMScf Michael Maeng MD, PhDf Thomas Engstrøm MD, PhDg Rune Wiseth MD, PhDh Jonas Persson MD, PhDi Thor Trovik MD, PhDj Ulf Jensen MD, PhDk Stefan K. James MD, PhDd Gary S. Mintz MDb Ovidiu Dressler MDb Aaron Crowley MAb OriBen-Yehuda MDbl David Erlinge MD, PhDm for the PROSPECT ABSORB Investigators Background Acute coronary syndromes most commonly arise from thrombosis of lipid-rich coronary atheromas that have large plaque burden despite angiographically appearing mild. Objectives This study sought to examine the outcomes of percutaneous coronary intervention (PCI) of non–flow-limiting vulnerable plaques. Methods Three-vessel imaging was performed with a combination intravascular ultrasound (IVUS) and near-infrared spectroscopy (NIRS) catheter after successful PCI of all flow-limiting coronary lesions in 898 patients presenting with myocardial infarction (MI). Patients with an angiographically nonobstructive stenosis not intended for PCI but with IVUS plaque burden of ≥65% were randomized to treatment of the lesion with a bioresorbable vascular scaffold (BVS) plus guideline-directed medical therapy (GDMT) versus GDMT alone. The primary powered effectiveness endpoint was the IVUS-derived minimum lumen area (MLA) at protocol-driven 25-month follow-up. The primary (nonpowered) safety endpoint was randomized target lesion failure (cardiac death, target vessel–related MI, or clinically driven target lesion revascularization) at 24 months. The secondary (nonpowered) clinical effectiveness endpoint was randomized lesion–related major adverse cardiac events (cardiac death, MI, unstable angina, or progressive angina) at latest follow-up. Results A total of 182 patients were randomized (93 BVS, 89 GDMT alone) at 15 centers. The median angiographic diameter stenosis of the randomized lesions was 41.6%; by near-infrared spectroscopy–IVUS, the median plaque burden was 73.7%, the median MLA was 2.9 mm2, and the median maximum lipid plaque content was 33.4%. Angiographic follow-up at 25 months was completed in 167 patients (91.8%), and the median clinical follow-up was 4.1 years. The follow-up MLA in BVS-treated lesions was 6.9 ± 2.6 mm2 compared with 3.0 ± 1.0 mm2 in GDMT alone–treated lesions (least square means difference: 3.9 mm2; 95% confidence interval: 3.3 to 4.5; p < 0.0001). Target lesion failure at 24 months occurred in similar rates of BVS-treated and GDMT alone–treated patients (4.3% vs. 4.5%; p = 0.96). Randomized lesion–related major adverse cardiac events occurred in 4.3% of BVS-treated patients versus 10.7% of GDMT alone–treated patients (odds ratio: 0.38; 95% confidence interval: 0.11 to 1.28; p = 0.12). Conclusions PCI of angiographically mild lesions with large plaque burden was safe, substantially enlarged the follow-up MLA, and was associated with favorable long-term clinical outcomes, warranting the performance of an adequately powered randomized trial. (PROSPECT ABSORB [Providing Regional Observations to Study Predictors of Events in the Coronary Tree II Combined with a Randomized, Controlled, Intervention Trial]; NCT02171065).

Reliability of Office, Home, and Ambulatory Blood Pressure Measurements and Correlation With Left Ventricular Mass Joseph E.Schwartz PhDab Paul Muntner PhDc Ian M. Kronish MDa Matthew M. Burg PhDd Thomas G. Pickering DPhil, MDa ∗John Thomas Bigger MDa∗ Daichi Shimbo MDa Background Determining the reliability and predictive validity of office blood pressure (OBP), ambulatory BP (ABP), and home BP (HBP) can inform which is best for diagnosing hypertension and estimating risk of cardiovascular disease. Objectives This study aimed to assess the reliability of OBP, HBP, and ABP and evaluate their associations with left ventricular mass index (LVMI) in untreated persons. Methods The Improving the Detection of Hypertension (IDH) study, a community-based observational study, enrolled 408 participants who had OBP assessed at 3 visits, and completed 3 weeks of HBP, 2 24-h ABP recordings, and a 2-dimensional echocardiogram. Mean age was 41.2 ± 13.1 years, 59.5% were women, 25.5% African American, and 64.0% Hispanic. Results The reliability of 1 week of HBP, 3 office visits with mercury sphygmomanometry, and 24-h ABP were 0.938, 0.894, and 0.846 for systolic and 0.918, 0.847, and 0.843 for diastolic BP, respectively. The correlations among OBP, HBP, and ABP, corrected for regression dilution bias, were 0.74 to 0.89. After multivariable adjustment including OBP and 24-h ABP, 10 mm Hg higher systolic and diastolic HBP were associated with 5.07 (standard error [SE]: 1.48) and 3.92 (SE: 2.14) g/m2 higher LVMI, respectively. After adjustment for HBP, neither systolic or diastolic OBP nor ABP was associated with LVMI. Conclusions OBP, HBP, and ABP assess somewhat distinct parameters. Compared with OBP (3 visits) or 24-h ABP, systolic and diastolic HBP (1 week) were more reliable and more strongly associated with LVMI. These data suggest that 1 week of HBP monitoring may be the best approach for diagnosing hypertension.

Sleep Irregularity and Risk of Cardiovascular Events: The Multi-Ethnic Study of Atherosclerosis Tianyi Huang ScD, MSca Sara Mariani PhDb Susan Redline MD, MPHb Background The cardiovascular system exhibits strong circadian rhythms to maintain normal functioning. Irregular sleep schedules, characterized by high day-to-day variability in sleep duration or timing, represent possibly milder but much more common and chronic disruption of circadian rhythms in the general population than shift work. Objectives This study aimed to prospectively examine the association between sleep regularity and risk of cardiovascular disease (CVD). Methods In MESA (Multi-Ethnic Study of Atherosclerosis), 1,992 participants free of CVD completed 7-day wrist actigraphy for sleep assessment from 2010 to 2013 and were prospectively followed through 2016. The study assessed sleep regularity using the SD of actigraphy-measured sleep duration and sleep-onset timing across 7 days. Incident CVD included nonfatal and fatal cardiovascular events. A Cox proportional hazards model was used to estimate hazard ratios (HRs) for incident CVD according to SD of sleep duration and timing, adjusted for traditional CVD risk factors (including CVD biomarkers) and other sleep-related factors (including average sleep duration). Results During a median follow-up of 4.9 years, 111 participants developed CVD events. The multivariable-adjusted HRs (95% confidence intervals) for CVD across categories of sleep duration SD were 1.00 (reference) for ≤60 min, 1.09 (0.62 to 1.92) for 61 to 90 min, 1.59 (0.91 to 2.76) for 91 to 120 min, and 2.14 (1.24 to 3.68) for >120 min (p trend = 0.002). Similarly, compared with participants with a sleep timing SD ≤30 min, the HRs (95% confidence intervals) for CVD were 1.16 (0.64 to 2.13) for 31 to 60 min, 1.52 (0.81 to 2.88) for 61 to 90 min, and 2.11 (1.13 to 3.91) for >90 min (p trend = 0.002). Exclusion of current shift workers yielded similar results. Conclusions Irregular sleep duration and timing may be novel risk factors for CVD, independent of traditional CVD risk factors and sleep quantity and/or quality.

Saturated Fats and Health: A Reassessment and Proposal for Food-Based Recommendations: JACC State-of-the-Art Review Arne Astrup MD, DMSca Faidon Magkos PhDa Dennis M.Bier MDbJ. Thomas Brenna PhDcde Marcia C.de Oliveira Otto PhDf James O. Hill PhDg Janet C.King PhDh Andrew Mente Ph DiJose M. Ordovas PhDj Jeff S. Volek PhD, RDk Salim Yusuf DPhili Ronald M. Krauss MDlm The recommendation to limit dietary saturated fatty acid (SFA) intake has persisted despite mounting evidence to the contrary. Most recent meta-analyses of randomized trials and observational studies found no beneficial effects of reducing SFA intake on cardiovascular disease (CVD) and total mortality, and instead found protective effects against stroke. Although SFAs increase low-density lipoprotein (LDL) cholesterol, in most individuals, this is not due to increasing levels of small, dense LDL particles, but rather larger LDL particles, which are much less strongly related to CVD risk. It is also apparent that the health effects of foods cannot be predicted by their content in any nutrient group without considering the overall macronutrient distribution. Whole-fat dairy, unprocessed meat, and dark chocolate are SFA-rich foods with a complex matrix that are not associated with increased risk of CVD. The totality of available evidence does not support further limiting the intake of such foods.

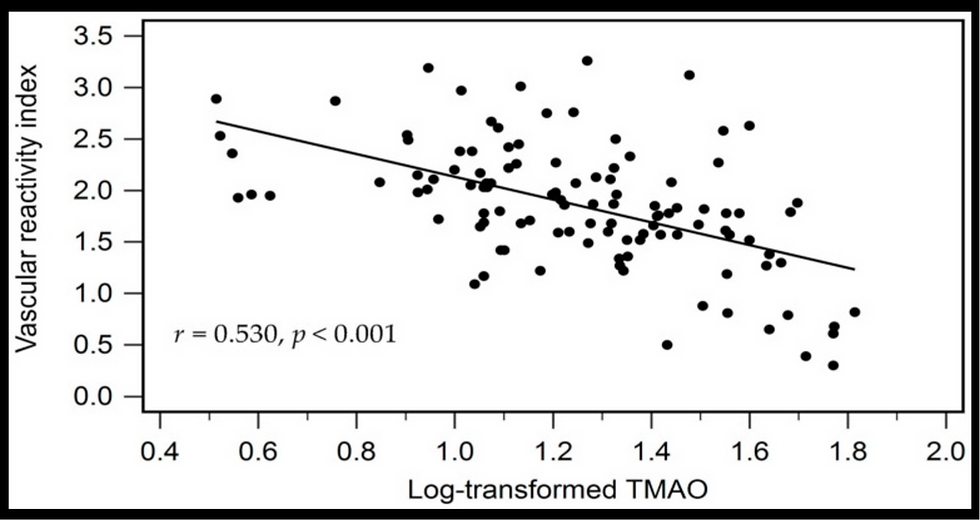
![Lipoprotein(a) levels predict endothelial dysfunction in maintenance hemodialysis patients: evidence from [VENDYS] vascular reactivity index assessment](https://static.wixstatic.com/media/dac531_5285607cc591409a9d83746f042af7c6~mv2.png/v1/fill/w_980,h_980,al_c,q_90,usm_0.66_1.00_0.01,enc_avif,quality_auto/dac531_5285607cc591409a9d83746f042af7c6~mv2.png)

Comments