Rheumatologists want a bigger seat at COVID research table,
- heartlung
- Jan 16, 2023
- 3 min read
Updated: Jan 18, 2023
pointing to COVID causing auto-immune diseases (linked to hyperinflammatory endothelial dysfunction)
Ann Rheum Dis 2021
EULAR points to consider on pathophysiology and use of immunomodulatory therapies in COVID-19
Alessia Alunno # 1, Aurélie Najm # 2, Pedro M Machado 3 4 5, Heidi Bertheussen 6, Gerd R Burmester 7, Francesco Carubbi 8, Gabriele De Marco 9, Roberto Giacomelli 10, Olivier Hermine 11 12, John D Isaacs 13, Isabelle Koné-Paut 14, César Magro-Checa 15, Iain McInnes 2, Pier Luigi Meroni 16, Luca Quartuccio 17, Athimalaipet V Ramanan 18 19, Manuel Ramos-Casals 20, Javier Rodríguez Carrio 21, Hendrik Schulze-Koops 22, Tanja A Stamm 23, Sander W Tas 24, Benjamin Terrier 25, Dennis G McGonagle 9, Xavier Mariette 26
Affiliations
1Rheumatology Unit, Department of Medicine, University of Perugia, Perugia, Italy.
2 Institute of Infection, Immunity and Inflammation, College of Medical Veterinary and Life Sciences, University of Glasgow, Glasgow, UK.
3 Centre for Rheumatology & Department of Neuromuscular Diseases, University College London, London, UK.
4 National Institute for Health Research (NIHR) Biomedical Research Centre (BRC), University College London Hospitals NHS Foundation Trust, London, UK.
5 Department of Rheumatology, Northwick Park Hospital, London North West University Healthcare NHS Trust, London, UK.
6 Oslo, Norway.
7 Department of Rheumatology and Clinical Immunology, Charité – Universitätsmedizin Berlin, Freie Universität und Humboldt-Universität Berlin, Berlin, Germany.
8 Department of Medicine, ASL 1 Avezzano-Sulmona-L’Aquila, Internal Medicine and Nephrology Unit, Department of Life, Health & Environmental Sciences, University of L’Aquila, L’Aquila, Italy.
9 The Leeds Institute of Rheumatic and Musculoskeletal Medicine, University of Leeds, Leeds, UK.
10 Rheumatology and Clinical Immunology Unit, University of Rome “Campus Biomedico” School of Medicine Rome, Rome, Italy.
11 Department of Haematology, Hôpital Necker, Assistance Publique – Hôpitaux de Paris, Paris, France.
12 INSERM UMR1183, Institut Imagine, Université de Paris, Paris, France.
13 Translational and Clinical Research Institute, Newcastle University and Musculoskeletal Unit, Newcastle Hospitals NHS Foundation Trust, Newcastle upon Tyne, UK.
14 Service de Rhumatologie Pédiatrique, Centre de Référence des Maladies Auto-Inflammatoires de l’enfant, Hôpital Bicêtre, AP HP, Université Paris Sud, Bicètre, France.
15 Department of Rheumatology, Zuyderland Medical Centre Heerlen, Heerlen, The Netherlands.
16 Experimental Laboratory of Immunological and Rheumatologic Researches, Istituto Auxologico Italiano, IRCCS, Milan, Italy.
17 Department of Medicine, Rheumatology Clinic, University of Udine, ASUFC Udine, Udine, Italy.
18 University Hospitals Bristol NHS Foundation Trust, Bristol, UK.
19 University of Bristol Translational Health Sciences, Bristol, UK.
20 Department of Autoimmune Diseases, ICMiD, Laboratory of Autoimmune Diseases Josep Font, IDIBAPS-CELLEX, Department of Autoimmune Diseases, ICMiD, University of Barcelona, Hospital Clínic, Barcelona, Spain.
21 Department of Functional Biology, Immunology Area, Faculty of Medicine, University of Oviedo, Instituto de Investigación Sanitaria del Principado de Asturias (ISPA), Oviedo, Spain.
22 Division of Rheumatology and Clinical Immunology, Department of Internal Medicine IV, Ludwig-Maximilians University of Munich, Munchen, Germany.
23 Section for Outcomes Research, Center for Medical Statistics, Informatics, and Intelligent Systems, Medical University of Vienna and Ludwig Boltzmann Institute for Arthritis and Rehabilitation, Wien, Austria.
24 Department of Rheumatology and Clinical Immunology, Amsterdam Rheumatology and Immunology Center, Amsterdam University Medical Centres, Amsterdam, The Netherlands.
25 Department of Internal Medicine, Cochin University Hospital, Paris, France; National Referral Centre for Systemic and Autoimmune Diseases, University Paris Descartes, Sorbonne Paris Cité, Paris, France.
26 Assistance Publique-Hôpitaux de Paris, Hôpital Bicêtre, INSERM UMR1184, Department of Rheumatology, Université Paris-Saclay, Le Kremlin Bicêtre, France xavier.mariette@aphp.fr.
Abstract Objectives: Severe systemic inflammation associated with some stages of COVID-19 and in fatal cases led therapeutic agents developed or used frequently in Rheumatology being at the vanguard of experimental therapeutics strategies. The aim of this project was to elaborate EULAR Points to consider (PtCs) on COVID-19 pathophysiology and immunomodulatory therapies. Methods: PtCs were developed in accordance with EULAR standard operating procedures for endorsed recommendations, led by an international multidisciplinary Task Force, including rheumatologists, translational immunologists, haematologists, paediatricians, patients and health professionals, based on a systemic literature review up to 15 December 2020. Overarching principles (OPs) and PtCs were formulated and consolidated by formal voting. Results: Two OPs and fourteen PtCs were developed. OPs highlight the heterogeneous clinical spectrum of SARS-CoV-2 infection and the need of a multifaceted approach to target the different pathophysiological mechanisms. PtCs 1-6 encompass the pathophysiology of SARS-CoV-2 including immune response, endothelial dysfunction and biomarkers. PtCs 7-14 focus on the management of SARS-CoV-2 infection with immunomodulators. There was evidence supporting the use of glucocorticoids, especially dexamethasone, in COVID-19 cases requiring oxygen therapy. No other immunomodulator demonstrated efficacy on mortality to date, with however inconsistent results for tocilizumab. Immunomodulatory therapy was not associated with higher infection rates. Conclusions: Multifactorial pathophysiological mechanisms, including immune abnormalities, play a key role in COVID-19. The efficacy of glucocorticoids in cases requiring oxygen therapy suggests that immunomodulatory treatment might be effective in COVID-19 subsets. Involvement of rheumatologists, as systemic inflammatory diseases experts, should continue in ongoing clinical trials delineating optimal immunomodulatory therapy utilisation in COVID-19. Keywords: immune system diseases; inflammation; therapeutics.

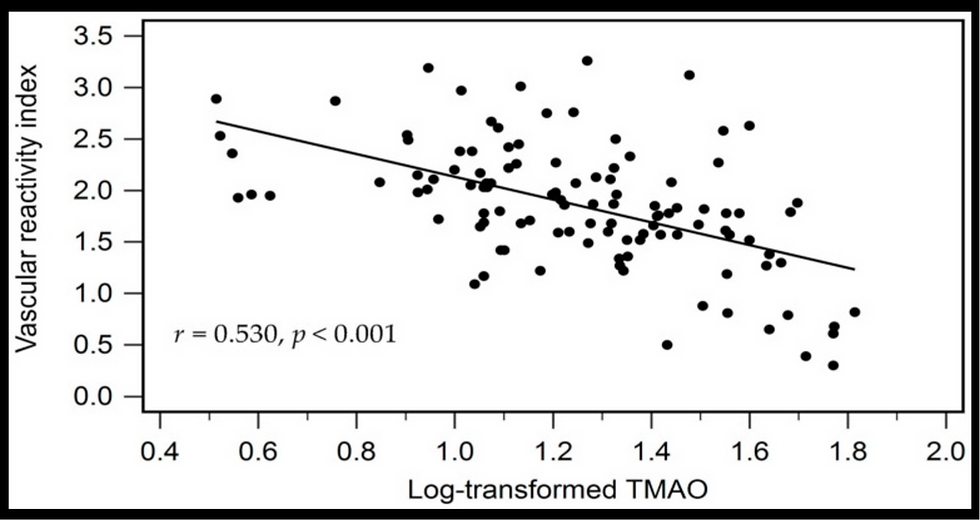
![Lipoprotein(a) levels predict endothelial dysfunction in maintenance hemodialysis patients: evidence from [VENDYS] vascular reactivity index assessment](https://static.wixstatic.com/media/dac531_5285607cc591409a9d83746f042af7c6~mv2.png/v1/fill/w_980,h_980,al_c,q_90,usm_0.66_1.00_0.01,enc_avif,quality_auto/dac531_5285607cc591409a9d83746f042af7c6~mv2.png)

Comments