SARS-CoV2: should inhibitors of the renin–angiotensin system be withdrawn in patients with COVID-19?
- heartlung
- Jan 16, 2023
- 5 min read
In a rapid response published online by the British Medical Journal, Sommerstein and Gräni1 pushed forward the hypothesis that angiotensin-converting enzyme (ACE) inhibitors (ACE-Is) could act as a potential risk factor for fatal Corona virus disease 2019 (COVID-19) by up-regulating ACE2. This notion was quickly picked up by the lay press and sparked concerns among physicians and patients regarding the intake of inhibitors of the renin–angiotensin–aldosterone system (RAAS) by severe acute respiratory syndrome coronavirus 2 (SARS-CoV2) infected individuals.1 In this article, we try to shed light on what is known and unknown regarding the RAAS and SARS-CoV2 interaction. We find translational evidence for diverse roles of the RAAS, which allows to formulate also the opposite hypothesis, i.e. that inhibition of the RAAS might be protective in COVID-19.
As of March 11, 124 910 patients worldwide have been tested positive for COVID-19 with a reported death toll amounting to 4589 patients, and the numbers continue to rise.2 First analyses of patient characteristics from China showed that diabetes, hypertension, and cardiovascular diseases are highly prevalent among SARS-CoV2 infected patients, and may be associated with poor outcome.3 Specifically, their prevalence was roughly three- to four-fold increased among patients reaching the combined primary endpoint of admission to an intensive care unit, mechanical ventilation, or death compared to patients with less severe outcomes. In general, patients with these conditions are frequently treated with inhibitors of the RAAS, namely ACE-Is, angiotensin II type 1 receptor blockers (ARBs), or mineralocorticoid receptor antagonists (MRAs).
As previously shown for SARS-CoV,4 SARS-CoV25 similarly utilizes ACE2 as receptor for viral cell entry. In the RAAS, ACE2 catalyses the conversion of angiotensin II to angiotensin 1–7, which acts as a vasodilator and exerts protective effects in the cardiovascular system. In animal experiments, increased expression and activity of ACE2 in various organs including the heart were found in connection with ACE-I and ARB administration.6 In addition, more recent data showing increased urinary secretion of ACE2 in hypertensive patients treated with the ARB olmesartan suggest that up-regulation of ACE2 may also occur in humans.7 These observations have been reiterated in the literature and on the web in recent days and the question arose whether RAAS inhibition may increase the risk of deleterious outcome of COVID-19 through up-regulation of ACE2 and increase of viral load.
Despite the possible up-regulation of ACE2 by RAAS inhibition and the theoretically associated risk of a higher susceptibility to infection, there is currently no data proving a causal relationship between ACE2 activity and SARS-CoV2 associated mortality. Furthermore, ACE2 expression may not necessarily correlate with the degree of infection. Although ACE2 is thought to be mandatory for SARS-CoV infection, absence of SARS-CoV was observed in some ACE2 expressing cell types, whereas infection was present in cells apparently lacking ACE2, suggesting that additional co-factors might be needed for efficient cellular infection.8 In addition, lethal outcome of COVID-19 is mostly driven by the severity of the underlying lung injury. Importantly, in a mouse model of SARS-CoV infection and pulmonary disease, a key pathophysiological role was shown for ACE, angiotensin II and angiotensin II receptor type 1.9 SARS-CoV or SARS-CoV spike protein led to down-regulation of ACE2 and more severe lung injury in mice that could be attenuated by administration of an ARB9,10 These findings suggest a protective role of ARB in SARS-CoV associated lung injury and give rise to the hypothesis that primary activation of the RAAS in cardiovascular patients, rather than its inhibition, renders them more prone to a deleterious outcome.11
It is important to note that Guan et al.3 do not report how many patients were taking ACE-Is or ARBs. Based on data from the China PEACE Million Persons Project, nearly half of Chinese adults between 35 and 75 years are suffering from hypertension, but fewer than one third receive treatment, and blood pressure control is achieved in less than 10%.12 Furthermore, there is thus far no data showing that hypertension or diabetes are independent predictors of fatal outcome. Therefore, based on currently available data and statistics, the assumption of a causal relationship between ACE-I or ARB intake and deleterious outcome in COVID-19 is not legitimate. In fact, in a case of reverse causality, patients taking ACE-Is or ARBs may be more susceptible for viral infection and have higher mortality because they are older, more frequently hypertensive, diabetic, and/or having renal disease.
Conceptual figure highlighting the central role of ACE2 in the potentially deleterious (red) and protective (green) effects of the RAAS and its inhibition in the development of severe acute respiratory syndrome (SARS). ACE-Is and ARBs increase ACE2 expression and activity (grey) as shown by a few animal and human studies,6,7 but the mechanism has yet to be identified. Although there is currently no evidence, this could theoretically increase viral load and worsen outcome (red). In a reverse causality, ACE2 acts as a gatekeeper of the RAAS by degrading AngII to Ang1-7, hence diminishing its Ang II receptor 1-mediated deleterious effects. Therefore, ACE-I or ARB treatment could theoretically mitigate lung injury (green). Evidence for this mainly stems from animal studies.9,10 Providing soluble recombinant (r)ACE2 (blue) addresses both mechanisms by cell independent binding of SARS-CoV2 and degrading AngII to Ang 1-7. This concept is currently being tested in a pilot study in patients with COVID-19.13
Clearly, much more research is needed to clarify the multifaceted role of the RAAS in connection with SARS-CoV2 infection. Although there is data from animal studies suggesting potentially deleterious effects of the RAAS, prove-of-concept in humans is still lacking. Similarly, a few animal and human studies suggest up-regulation of ACE2 in response to RAAS inhibition through a yet to be identified mechanism, but whether this increases viral load in a critical way, and how viral load per se relates to disease severity remains unknown. Nevertheless, based on the work by Josef Penninger et al.,13 who proposed to therapeutically use the dual function of ACE2 as viral receptor and gatekeeper of RAAS activation, a pilot trial using soluble human recombinant ACE2 (APN01) in patients with COVID-19 has recently been initiated (Clinicaltrials.gov #NCT04287686). Such therapy could have the potential to lower both the viral load and the deleterious effects of angiotensin II activity.
In the meantime, we are well-advised to stick to what is known. There is abundant and solid evidence of the mortality-lowering effects of RAAS inhibitors in cardiovascular disease. ACE-Is, ARBs, and MRAs are the cornerstone of a prognostically beneficial heart failure therapy with the highest level of evidence with regard to mortality reduction.14 They all have in common the inhibition of the adverse cardiovascular effects arising from the interaction of angiotensin II with the angiotensin II receptor type 1. Discontinuation of heart failure therapy leads to deterioration of cardiac function and heart failure within days to weeks with a possible respective increase in mortality.15–17 Similarly, ACE-Is, ARBs, and MRAs are part of the standard therapy in hypertension18 and after myocardial infarction.19 Significant reduction of post-infarct mortality applies to all three substance classes, whereby early initiation of therapy (within days after infarction) is an important factor of success.20–23
In conclusion, based on currently available data and in view of the overwhelming evidence of mortality reduction in cardiovascular disease, ACE-I and ARB therapy should be maintained or initiated in patients with heart failure, hypertension, or myocardial infarction according to current guidelines as tolerated, irrespective of SARS-CoV2. Withdrawal of RAAS inhibition or preemptive switch to alternate drugs at this point seems not advisable, since it might even increase cardiovascular mortality in critically ill COVID-19 patients.
Source:
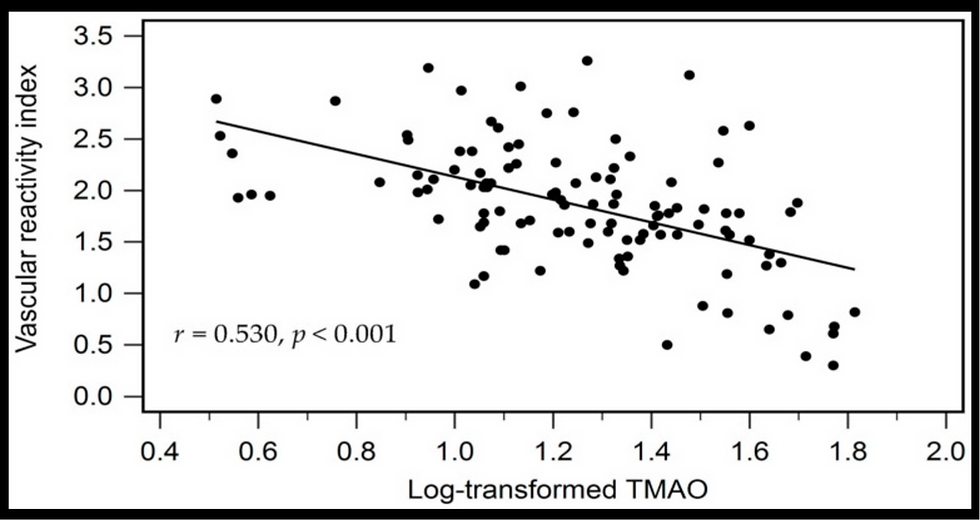
![Lipoprotein(a) levels predict endothelial dysfunction in maintenance hemodialysis patients: evidence from [VENDYS] vascular reactivity index assessment](https://static.wixstatic.com/media/dac531_5285607cc591409a9d83746f042af7c6~mv2.png/v1/fill/w_980,h_980,al_c,q_90,usm_0.66_1.00_0.01,enc_avif,quality_auto/dac531_5285607cc591409a9d83746f042af7c6~mv2.png)

Comments