Systemic vascular health is compromised in both confirmed and unconfirmed asthma
- heartlung
- Jan 16, 2023
- 2 min read
Updated: Jan 18, 2023
Systemic vascular health is compromised in both confirmed and unconfirmed asthma Shelby L Henry 1, Linn E Moore 2, Andrew R Brotto 2, Samira Rowland 2, Desi Fuhr 2, Michael K Stickland 3
Affiliations
1 Pulmonary Division, Department of Medicine, Faculty of Medicine and Dentistry, University of Alberta, Canada; Faculty of Rehabilitation Medicine, University of Alberta, Edmonton, Alberta, Canada.
2 Pulmonary Division, Department of Medicine, Faculty of Medicine and Dentistry, University of Alberta, Canada.
3 Pulmonary Division, Department of Medicine, Faculty of Medicine and Dentistry, University of Alberta, Canada. Electronic address: michael.stickland@ualberta.ca.
Abstract Introduction: Asthma is associated with increased risk of cardiovascular diseases. Despite many presenting with symptoms of asthma, asthma cannot always be confirmed by physiological assessment. It is thus far unknown if the heightened cardiovascular risk applies to this group. The purpose of this study was to examine markers of cardiovascular risk, including endothelial function, arterial stiffness, and systemic inflammation, in individuals with confirmed asthma, unconfirmed asthma, and healthy controls. As short-acting beta agonist (SABA) use is associated with increased cardiovascular risk, a secondary analysis was conducted to investigate the impact of regular SABA use on vascular outcomes. Methods: Individuals with confirmed asthma (n = 26), unconfirmed asthma (n = 15), and healthy controls (n = 26) were recruited for this cross-sectional study. Asthma was confirmed by FEV1 reversibility, methacholine challenge, or exercise challenge. Endothelial function was assessed using flow-mediated dilation (FMD), arterial stiffness using pulse wave velocity (PWV), and systemic inflammation by C-reactive protein (CRP) levels. Results: FMD was significantly lower in both asthma groups compared to controls (confirmed: 7.7 ± 3.6%, unconfirmed: 7.3 ± 3.5%, controls: 10.4 ± 3.6%, p = 0.02). No difference was found in PWV nor CRP. Asthma participants who used SABA had increased arterial stiffness compared to those without SABA (9.2 ± 2.7 m/s, 7.7 ± 1.1 m/s respectively, p = 0.03). No difference was seen in FMD or CRP between SABA groups. Conclusion: Individuals with a clinical history of asthma symptoms demonstrate vascular impairments regardless of physiological confirmation of disease. Regular SABA use increases arterial stiffness. Avoiding potentially inappropriate SABA use among people without physiologically confirmed asthma may thus be beneficial in curbing cardiovascular risk. Keywords: Arterial stiffness; Asthma; Cardiovascular; Flow-mediated dilation; Short-acting beta agonist; Vascular function.

Vascular outcomes compared between healthy controls, unconfirmed asthma, and confirmed asthma. FMD: Flow-mediated dilation [a measure of macrovascular endothelial function].
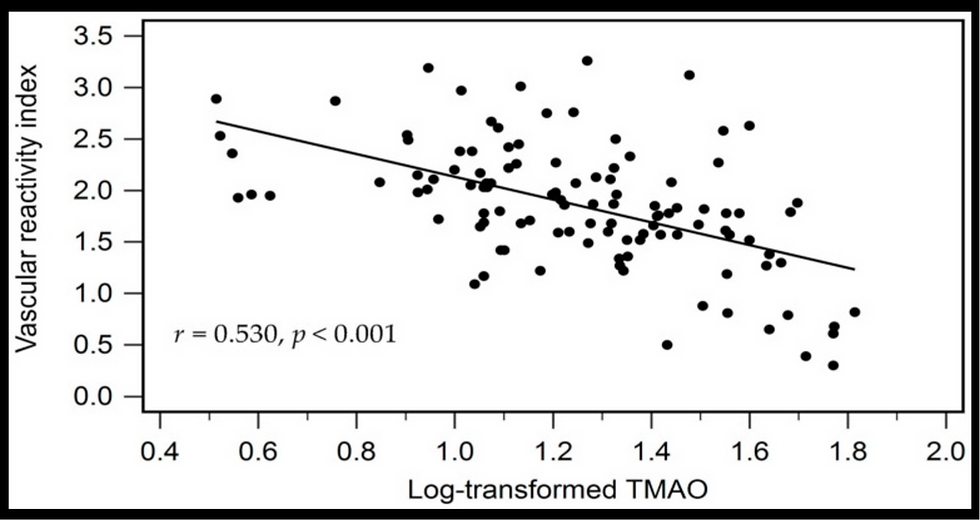
![Lipoprotein(a) levels predict endothelial dysfunction in maintenance hemodialysis patients: evidence from [VENDYS] vascular reactivity index assessment](https://static.wixstatic.com/media/dac531_5285607cc591409a9d83746f042af7c6~mv2.png/v1/fill/w_980,h_980,al_c,q_90,usm_0.66_1.00_0.01,enc_avif,quality_auto/dac531_5285607cc591409a9d83746f042af7c6~mv2.png)

Comments